In the United States, only 15% of available donor lungs are transplanted into critical recipients due to the associated damage to the organs from the traumatic death event.
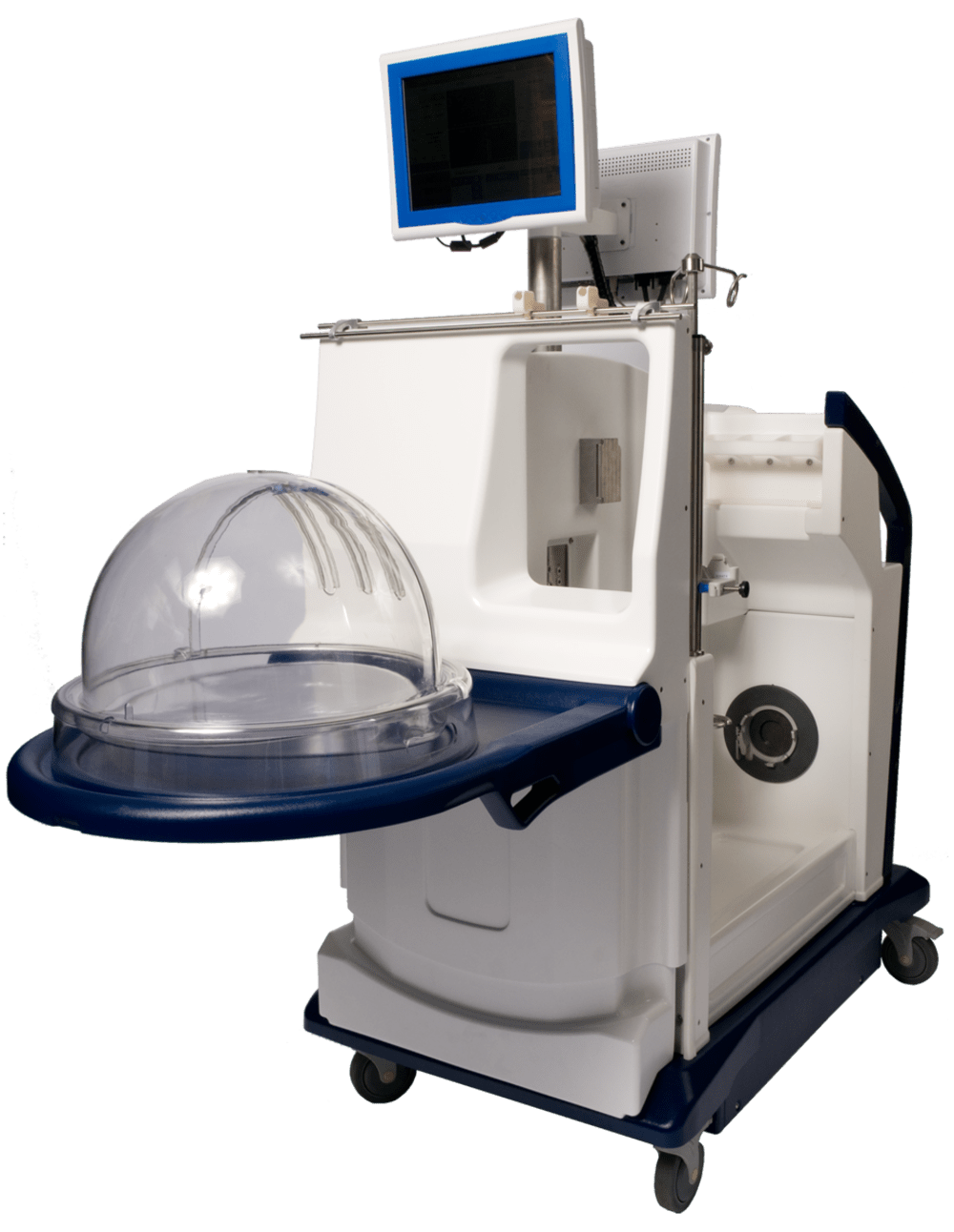
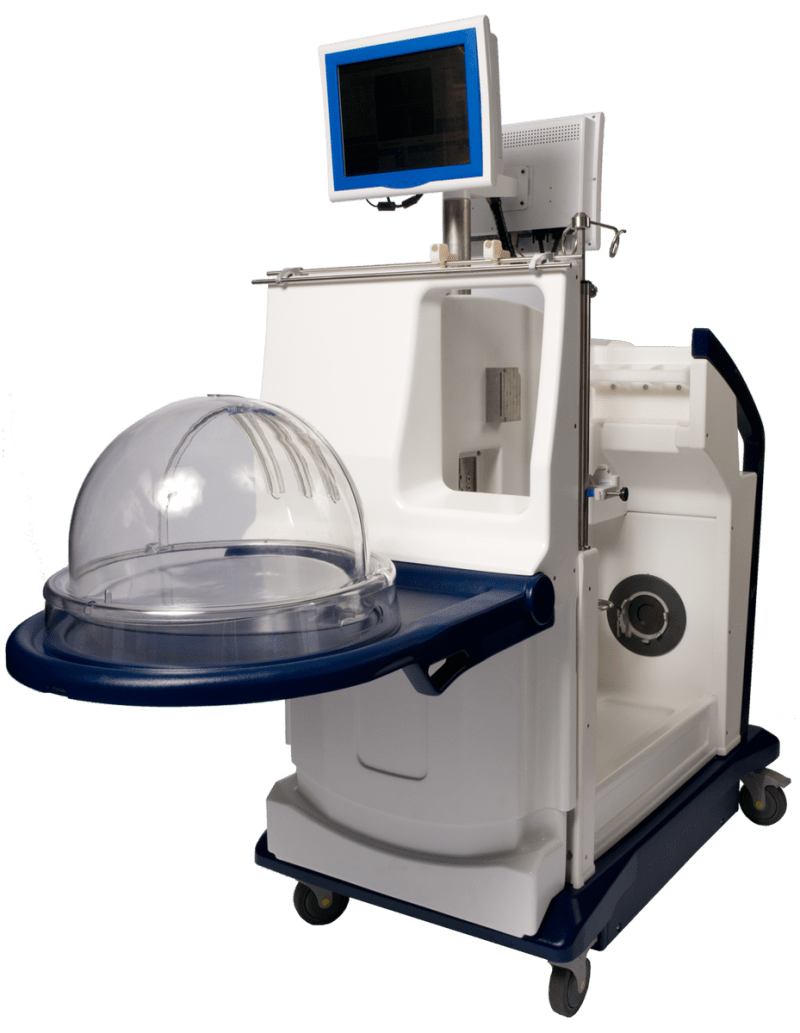
The XVIVO Perfusion System (XPS) is a mobile intensive care unit that can repair damaged organs ex vivo (out of the donor's body) for successful transplantation into a waiting recipient. The XPS includes a centrifugal cardiac bypass pump, fluid heater/cooler unit, in-line fiber optic gas analyzer (to determine continuous pH, pCO2 and pO2) and an ICU ventilator. It safely perfuses a blood substitute throughout the entire organ in a carefully controlled environment, which allows the damaged organ to effectively repair itself over time. In a North American clinical trial (published in April, 2011 in the New England Journal of Medicine), it was shown that 60% of available donor lungs can actually be used safely for transplant using our technique, an increase of 45% over current US numbers!
We have just started a US clinical trial in June, 2011, in persuit of FDA approval for the XPS device and technique to recondition human lungs for transplant. In the near future, we plan to extend our technique to additional donor organs, including liver, heart and kidney. By creating a safe, isolated environment for organ perfusion, it is very possible to imagine using the XPS device to perfuse diseased organs (cancer, Cystic Fibrosis, etc.) treating them with high-dose chemotherapy, gene therapy and eventually stem cells. In such an isolated envionment, there would be no harmful side effects to the patient from these aggressive therapies.
Our XPS device was designed to be manufactured using best-of-class, off-the-shelf equipment in an effort to bring the device to market as quickly and inexpensively as possible. Under this rapid design model, the XPS was designed, prototyped, manufactured and validated for clinical trials in approximately one year. The cost for the XPS is similar to purchasing the individual components separately from a number of different manufacturers, but the advantage is that all required equipment fits and works together inside one device.
Transplant hospitals will purchase the XPS for use in their operating rooms. The organ will be transported to the hospital using the current cost-effective cold storage transport methods. Once it arrives to the hospital, the transplant team will connect the organ to the XPS and gradually warm it up to body temperature, allowing the organ to operate at full metabolism and repair itself as if it were still in a body. An additional advantage of this procedure is that it dramatically increases the time the organ remains viable from 6 hours (cold transport only) to more than 20 hours (combined cold, XPS warm and more cold), allowing more time to find better-matched recipients and greatly increasing successful outcomes.
With the XPS machine and the XVIVO technique, we believe that the US waiting list will decrease from the currently 110,000 waiting patients to a more manageable waiting list, eventually providing organs to all waiting recipients.
-
Awards
-
 2011 Medical Category Winner
2011 Medical Category Winner
Like this entry?
-
About the Entrant
- Name:Chris Jaynes
- Type of entry:teamTeam members:Chris Jaynes
Tom Taccini
Tim Klug - Software used for this entry:SolidWorks
- Patent status:pending