Problem:
Retinopathy of Prematurity (ROP) is a disease that affects premature infants. It is the leading cause of childhood blindness. Although effective treatments exist, many infants are still at risk due to the small window of time for detection. The current standard of care consists of in-person, manual screening by a pediatric ophthalmologist. Unfortunately, the number of infants in need of screening far surpasses the availability of specifically trained ophthalmologists. Consequently, fewer than 30% of neonatal intensive care units (NICUs) worldwide have fully compliant ROP screening programs.
Current Solution:
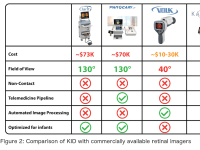
Telemedicine has been proposed as a possible solution to the screening deficit, but equipment and training costs present two major barriers to adoption. The current telemedicine standard is the RetCam, which is prohibitive due to high cost, complicated controls and lack of any telemedicine pipeline. RetCam is not designed for NICU incubators and its large and heavy form factor poses a risk of crushing infants if misused.
Other imagers fail to address the two greatest barriers to telemedicine adoption: cost and ease of use. In response, we have developed the Kaleyedos Imaging Device (KID).
Product Overview:
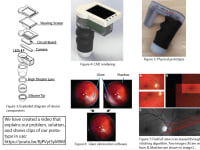
The KID streamlines the infant retinal imaging process, providing a low-cost, deskilled telemedicine solution to ROP. Our hardware component is a compact, wireless device specifically designed to be maneuverable in an infant incubator. The device itself contains a high-resolution camera, a non-contact, wide-field optical system with a specialized non-contact lens, and a novel illumination schema that works with our software suite to allow us to obtain high-quality retinal images at a much lower cost than currently available infant retinal imagers. Factoring in labor, production costs are less than $500 per unit, 10-20 times cheaper than production costs of competitors.
Our proprietary software component consists of a cloud server and an image processing suite. Images taken by the device are automatically uploaded to a cloud server where our software processes them, stores them, and makes them remotely accessible for grading from anywhere in the world. Our image processing suite uses computer vision concepts to aggregate images from our specialized optical system. Ultimately, we have been able to increase image quality and retinal field of view without additional hardware costs.
We have validated the device on medically relevant phantoms and are currently conducting our pilot human study at the Johns Hopkins Hospital.
Business Strategy:
We will begin marketing in the US where telemedicine provides an inexpensive and efficient solution for ROP screening. KID units are priced at $5,000 to undercut competition (priced at $30,000-75,000) and bypass administrative hospital purchasing boards, allowing us to market directly to end-user NICU clinicians and nurses through departmental purchasing channels. Another source of income will be software subscriptions, priced at $10,000 per hospital per year.
Impact:
Globally, up to 40% of premature infants develop ROP and around 10% of premature infants become blind within the first month. 490,000 infants are born blind each year. Our solution will not only drastically reduce the downstream costs of screening, but also prevent childhood blindness. worldwide
Video
-
Awards
-
 2017 Medical Honorable Mention
2017 Medical Honorable Mention -
 2017 Top 100 Entries
2017 Top 100 Entries
Like this entry?
-
About the Entrant
- Name:Elizabeth Wu
- Type of entry:teamTeam members:Erica Schwarz (team lead), Sami Messai, Becca Miller, Seony Han, Richard Chen, Aditya Murali, Prerna Singh
- Software used for this entry:Solidworks, Python, MatLab
- Patent status:pending