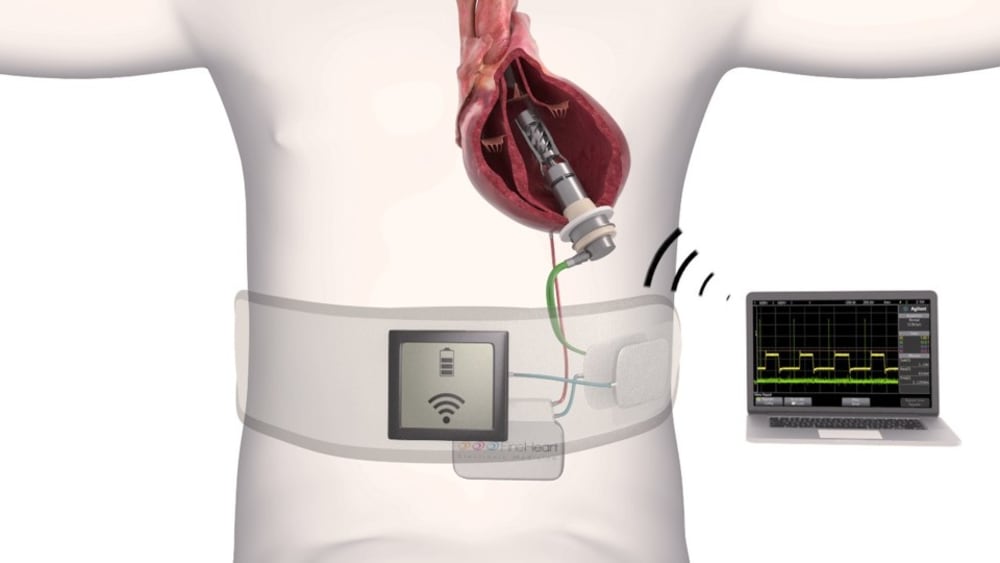
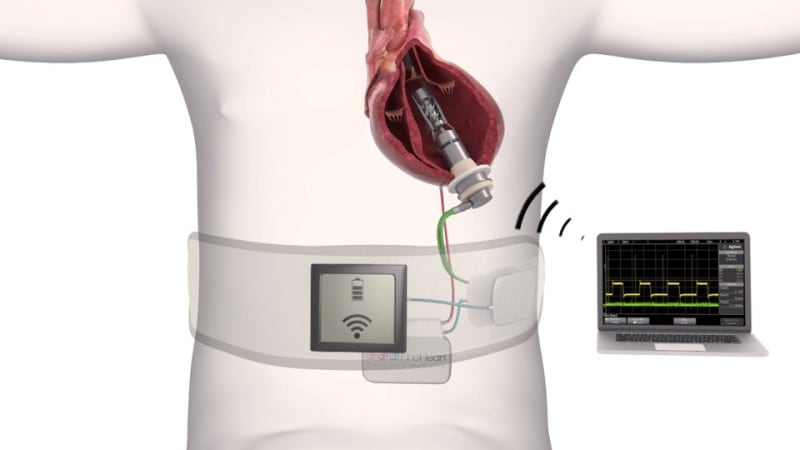
FineHeart has recently developed a device called the ICOMS FLOWMAKER. The Implantable Cardiac Output Management System (ICOMS) is an innovative hybrid between a pacemaker and a cardiac assist device. The technology was derived on a similar premise of cardiac resynchronization therapy (CRT), improving the heart’s rhythm, but targets the much larger patient population whose heart failure is mechanical, not electrical.
ICOMS is the first fully intraventricular flow accelerator providing pulsatile, physiologic support of the native heart function without bypassing the aorta. It respects the natural blood flow and is synchronized with the heart’s contractions – using the same technology as a pacemaker to track the heart’s contractions. No more than four inches long, ICOMS is the first miniaturized device with adjustable flow, allowing a physician to modify blood flow based on the patient’s heart failure severity.
Just as with the LVAD, ICOMS FLOWMAKER does not cure the heart, but the two technologies’ differences are profound. The entire ICOM system is fully implanted, eliminating the risk of driveline infection, a significant determinant of post-VAD morbidity and mortality. ICOMS respects the natural blood flow and heart contraction, and it is powered through the skin. Maintaining trans-aortic flow supports increased left ventricle unloading, improving myocardial recovery chances and faster device weaning possibilities. It is programmable, like a pacemaker, and the functioning mode can be customized for individual hemodynamic requirements, which preserves pump efficiency during arrhythmia and exercise.
From the patient perspective, it is designed to deliver improved quality of life by providing untethered freedom and supporting the patients’ return to daily activities such as exercising or simply enjoying a shower without worrying about protecting an external driveline.
With current technologies only offering temporary solutions, the ICOMS device fills a void in the management of patients, specifically those experiencing rolling cardiogenic shock. The ICOMS FLOWMAKER can be initiated as a temporary mechanical circulatory support (MCS) device and “morph” into lasting MCS if recovery doesn’t happen in the immediate term and can be explanted from a patient down the line if there is myocardial recovery.
In addition, promising therapeutic strategies focused on managing and treating comorbidities have proven beneficial for HF patients. Providing robust and long-term cardiac support, the ICOMS could facilitate clinicians’ ability to prescribe high doses of guideline-directed medical therapies, which have become substantially better in the past 5-10 years.
This modern approach, using ICOMS to facilitate high dose medical therapy, can drive higher recovery rates and provide more favorable cardiac reverse remodeling than what is seen in current practice with LVADs and temporary MCS devices
Video
-
Awards
-
 2021 Top 100 Entries
2021 Top 100 Entries
Like this entry?
-
About the Entrant
- Name:Victor Oribamise
- Type of entry:individual
- Patent status:pending