Whether you have acute back pain, a sports injury or the most common chronic condition, arthritis, you are almost guaranteed to develop some kind of musculoskeletal condition at some stage of your lives. In the case of the arthritis sufferers, a life-long sentence awaits them relieved only by pain-killers, steroids and infrequent and poorly accessible physiotherapy. Albeit temporary, sports injury and back pain sufferers are similarly incapacitated by pain and reduced mobility affecting work and day to day living. Typically physiotherapists will employ therapeutic ultrasound which has been used since the 1950’s due to its proven efficacy. These are large hand-held devices that require continuous movement for the treatment period, e.g. 20-30 minutes, causing operator fatigue, poor area coverage and therefore thermal hot-spots. Such devices are also handicapped by single frequency emission and by having small effective treatment areas.
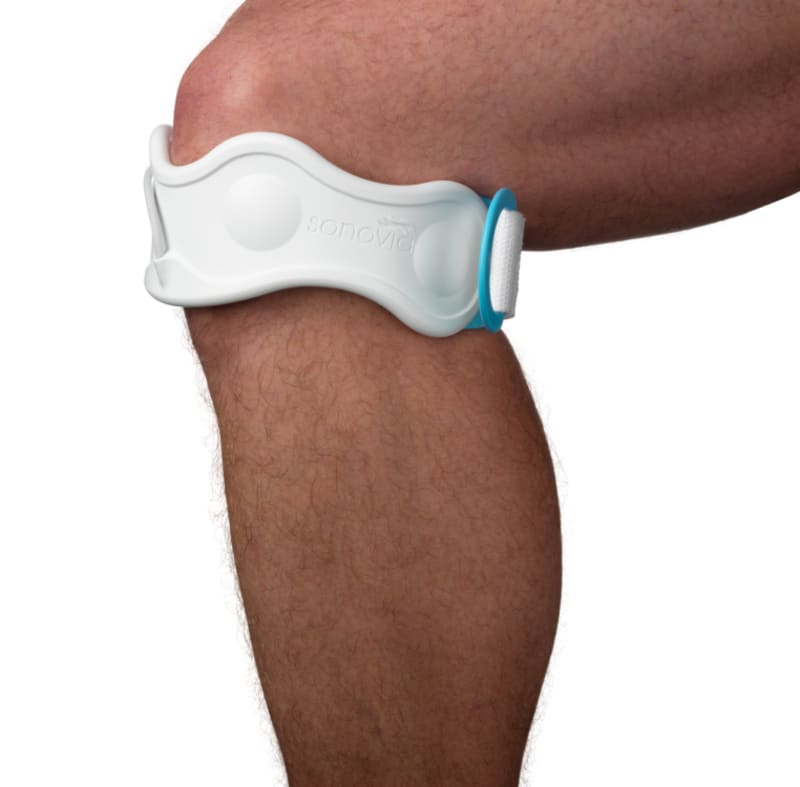
To overcome these limitations Sonovia has developed and patent-protected a new generation of therapeutic ultrasound device that can be used daily in the comfort of the patient’s home. Sonovia is developing an easy-on/easy-off joint support bandage that integrates multiple groups of miniaturised ultrasonic transducers. Once positioned, these groups are electronically activated in sequence along the bandage to produce a moving ultrasound ‘field’ around the circumference of the joint or limb. A small rechargeable battery-powered drive unit which controls this ultrasonic ‘movement’ also automatically limits the time per treatment enabling simple and safe operation by the patient. Numerical simulations of the depth of ultrasound propagation have also confirmed that ultrasound energy reaches sufficient depths to have orthopaedic efficacy. The bandage emits multiple frequencies thereby maximizing targeted therapy and also localized transdermal drug delivery (sonophoresis). Achieving this latter effect opens up the possibility of using analgesic-containing gels to couple the energy across to the skin to target localised pain and avoid the need to take oral NSAIDs or steroids which can trigger gastrointestinal complications.
The potential benefits to the healthcare system are far-reaching; the burden on hospitals for repeat treatments is reduced and the likelihood of late-stage joint degeneration requiring costly replacement surgery is also reduced. Additionally patients’ quality of life is improved through reduced pain and increased mobility and also because home-based self-care reduces patient inconvenience and expense due to reduced travel to and from clinics. Commercially this could be of considerable interest to medical device companies, healthcare companies/insurers and to pharmaceutical companies who need better efficacy of pain and inflammation targeting medicines.
Like this entry?
-
About the Entrant
- Name:Peter Luebcke
- Type of entry:individual
- Patent status:pending