Researchers at the University of Arizona are developing a COVID-19 testing method that uses a smartphone microscope to analyze saliva samples and deliver results in about 10 minutes, at the accuracy of detecting a single virus copy. The UArizona research team, led by biomedical engineering professor Jeong-Yeol Yoon, aims to combine the speed of existing nasal swab antigen tests with the high accuracy of nasal swab PCR, or polymerase chain reaction, tests.
The researchers are adapting an inexpensive method that they originally created to detect norovirus – the microbe famous for spreading on cruise ships – using a smartphone microscope. They plan to use the method in conjunction with a saline swish-gargle test developed by Michael Worobey at UArizona. The team's latest research using water samples – done in collaboration with Kelly A. Reynolds at UArizona – has recently been published in Nature Protocols. The team has worked to develop the smartphone-based COVID-19 detection method. They also remarked, "I have a couple of friends who had COVID-19 that were super frustrated, because their PCR results were taking six or seven days or they were getting false negatives from rapid antigen tests. But when they got the final PCR tests, they found out they had been sick, like they'd suspected. It's really cool to be working on a detection platform that can get fast results that are also accurate."
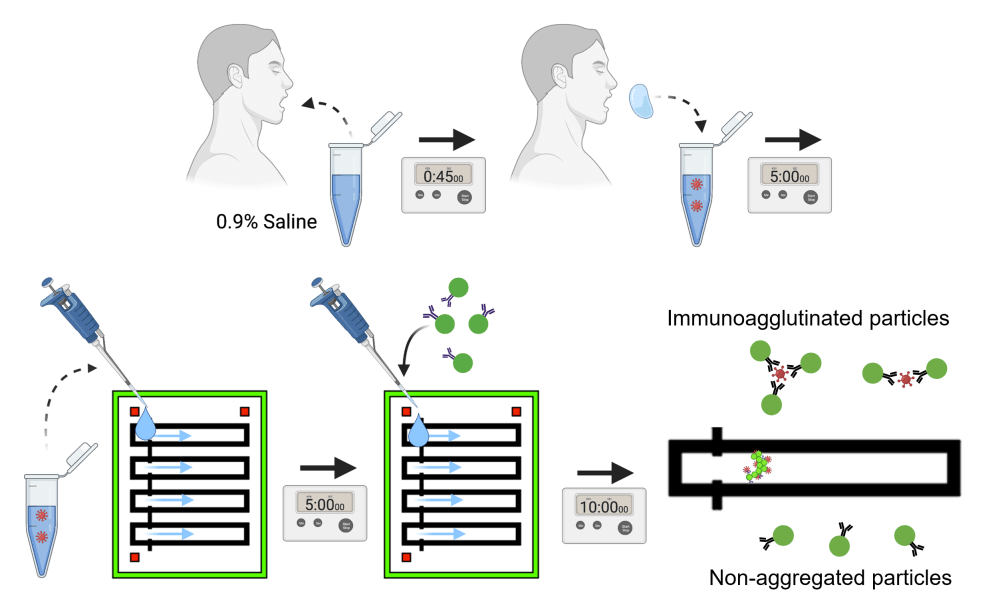
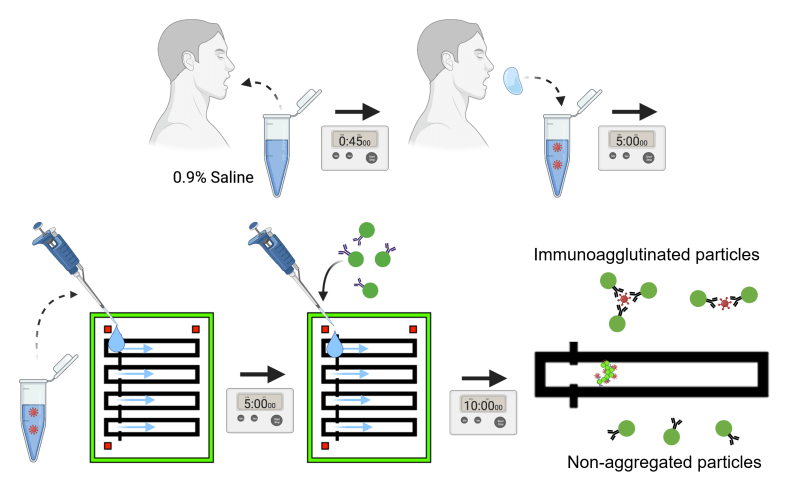
Traditional methods for detection of norovirus or other pathogens are often expensive, involve a large suite of laboratory equipment or require scientific expertise. The smartphone-based norovirus test developed at UArizona consists of a smartphone, a simple microscope and a piece of microfluidic paper – a wax-coated paper that guides the liquid sample to flow through specific channels. It is smaller and cheaper than other tests, with the components costing about $45. The basis of the technology is relatively simple. Users introduce antibodies with fluorescent beads to a water or saliva sample. If enough particles of the pathogen are present in the sample, several antibodies attach to each pathogen particle. Under a microscope, the pathogen particles show up as little clumps of fluorescent beads, which the user can then count. The process – adding beads to the sample, soaking a piece of paper in the sample, then taking a smartphone photograph of it under a microscope and counting the beads – takes about 10 minutes. It's so simple that a nonscientist could learn how to do it by watching a brief video.
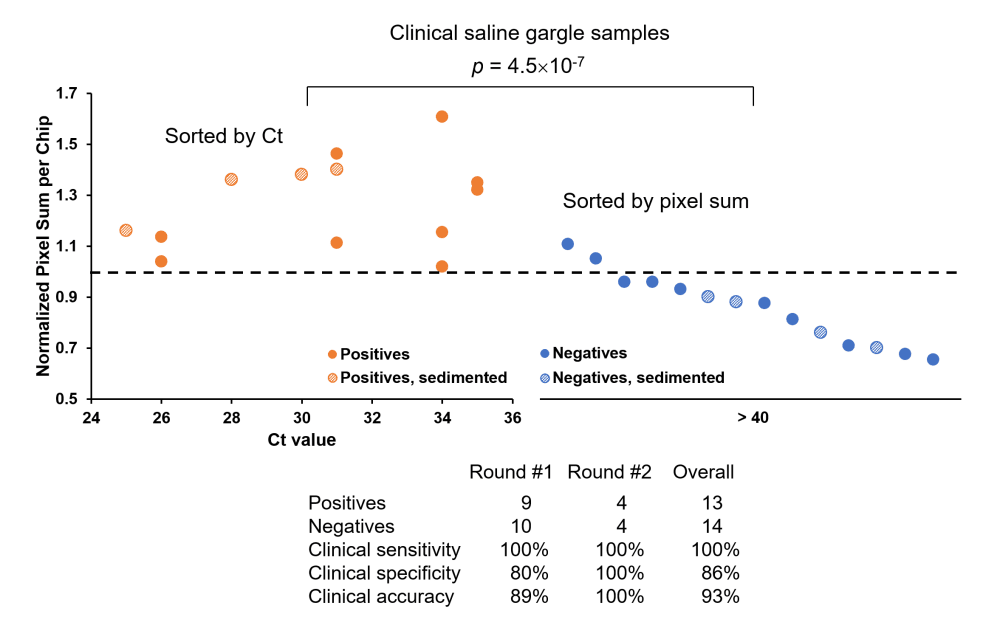
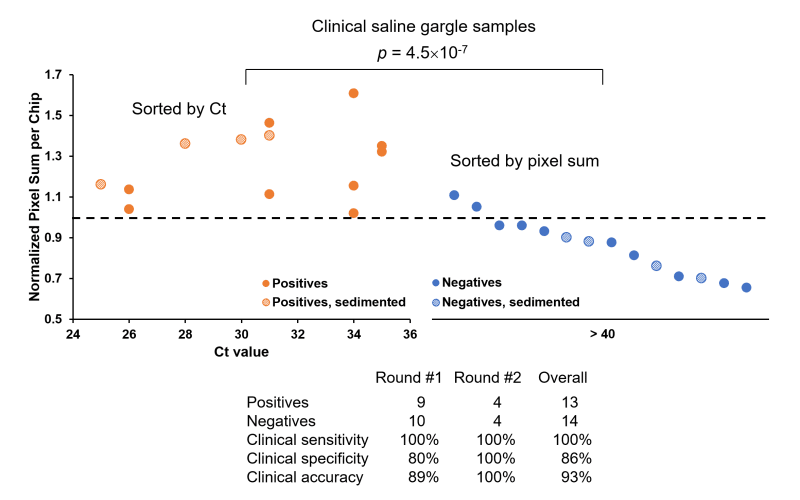
This promising technology could allow us to provide fast, accurate, affordable tests to the campus community frequently and easily. It will have a broader impact in mitigating the spread of the disease. The COVID-19 assay results from human clinical samples have recently been published in the PNAS Nexus (https://doi.org/10.1093/pnasnexus/pgac028). ABC TV's coverage can also be found at: https://www.abc15.com/news/coronavirus/ua-researchers-working-on-smartphone-test-for-covid-19
-
Awards
-
 2022 Electronics/Sensors/IoT Honorable Mention
2022 Electronics/Sensors/IoT Honorable Mention -
 2022 Top 100 Entries
2022 Top 100 Entries
Like this entry?
-
About the Entrant
- Name:Jeong Yeol Yoon
- Type of entry:individual
- Software used for this entry:SolidWorks, ImageJ
- Patent status:pending